Wedge biopsies are preferably obtained from at least 2 lobes with distinct radiographic involvement. A surgical lung biopsy is often required to make a definitive diagnosis. It can help rule out alternative diagnoses. Transbronchial lung biopsies may be attempted but are often inadequate to make a definitive diagnosis due to the small amount of lung tissue obtained and loss of tissue architecture from crush artifact. Marked elevation of eosinophils (greater than 25%) suggests eosinophilic pneumonia or rarely an overlap phenomenon. Lack of lymphocytosis on BAL portends a poor prognosis. Significant lymphocyte elevation (approximately 40%) is typical, and CD4/CD8 ratio reveals CD8 predominance. 
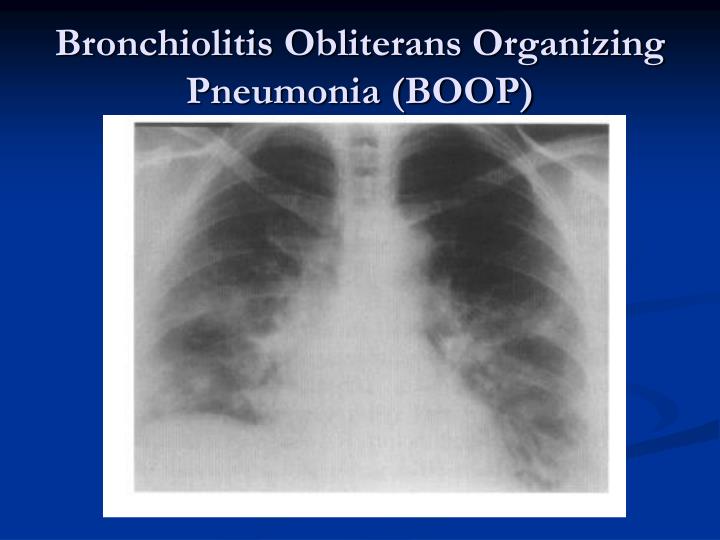
BAL fluid characteristically has mixed cellularity with neutrophils, lymphocytes, and eosinophils. Desaturation with 6-minute walk testing is also commonly noted.įlexible bronchoscopy with bronchoalveolar lavage (BAL) is often performed to rule out infections, pulmonary hemorrhage, and malignancy. PFTs typically reveal a restrictive defect with diffusion impairment. Multiple nodules and cavitary lesions should raise suspicion for malignancy. Other less common findings include irregular nodular opacities, cavitary lesions, and pleural effusions. This sign, seen in about 20% of patients with COP and is non-specific as it can be seen in various other infectious and inflammatory conditions. This sign is characterized by a dense outer rim of consolidation around a focal ground-glass opacity. The classic HRCT sign described in COP is the atoll sign, also known as the reverse halo sign. HRCT of the lungs reveals bilateral patchy peripherally located consolidations or ground glass opacities. High-Resolution Computed Tomography (HRCT) Other described findings include migratory, irregular, linear, or nodular opacities. The chest radiograph findings in COP include patchy diffuse consolidations mostly involving bilateral lower zones. When COP is suspected then testing for autoimmune diseases should be undertaken. Inflammatory markers, erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP), are commonly elevated. White cell count is typically elevated with neutrophilia. In experimental models, glucocorticoids have been shown to inhibit the formation of the granulation tissue plugs. Matrix metalloproteinases are also up-regulated. Vascular endothelial growth factor (VEGF) and basic fibroblast growth factor play a central role in organizing pneumonia. The third stage is an organization of fibroblasts and connective tissue matrix. Meanwhile, the alveolar cells proliferate and re-epithelialize the basal lamina, restoring the alveolar basement membrane. The second stage is characterized by proliferation of fibroblasts that lay down a reticulin framework. The intra-alveolar stage is comprised of formation of bands of fibrin along with infiltration of mononuclear inflammatory cells. The subsequent process of organization occurs in 3 stages. The other parts of the lungs like airways and blood vessels can also get affected.Pathogenic mechanisms have not been clearly described, but alveolar epithelial injury due to an unknown provocative insult is thought to cause leakage of plasma proteins into the alveolar space resulting in recruitment of inflammatory cells. Therefore, the person experiences shortness of breath and persistent dry cough, as a consequence of labored breathing. As a result, one faces difficulty in inhaling the air and hence the lungs cannot expand fully. However, if this process gets affected, too much tissue is formed, which then covers the entire lung and forms a thick scar over the lung. Normally, our body produces the needed amount of tissue for healing in response to any injury. The thickening of the tissue results due to scarring, inflammation or edema (fluid collection). This normal functioning of the air sacs gets impaired due to the thickening of the tissue of alveoli. They facilitate the exchange of gases between the lungs and the blood. This network acts as a protection for the air sacs or alveoli. It is so thin that it is not normally visible in an x-ray or CT scan. Interstitium is a very thin, lacy network that runs all over the lungs. All of them show the same physical presentation- thickening of the interstitium (the tissue and space lining the air sacs). Interstitial lung disease (ILD) is not a single condition, but a group of different diseases.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
